When starting a new contraception, it’s important to follow a few simple rules for success and make sure everything’s working smoothly. We spoke to Dr Desiree Gambushe, a medical doctor with Zoie Health, and got her advice for when you want to make a switch.
Here’s what she wants you to know before starting your new contraception method:
Before choosing a new contraception, get a health profile
Before starting a new contraception, it’s important to let your doctor know about your risk factors, what other medication you’re on and any family medical history, like diabetes, heart disease and any other diseases so that your doctor can assess the possible impacts your medication can have.
“There are side-effects to almost all, if not all medications,” says “So you do not want to start anyone on a medication that will possibly be harmful to them.”
Hormonal contraception like the pill, patch, injection, contain estrogen-like hormones which have similar effects on the body to those of the naturally-produced version of those hormones.
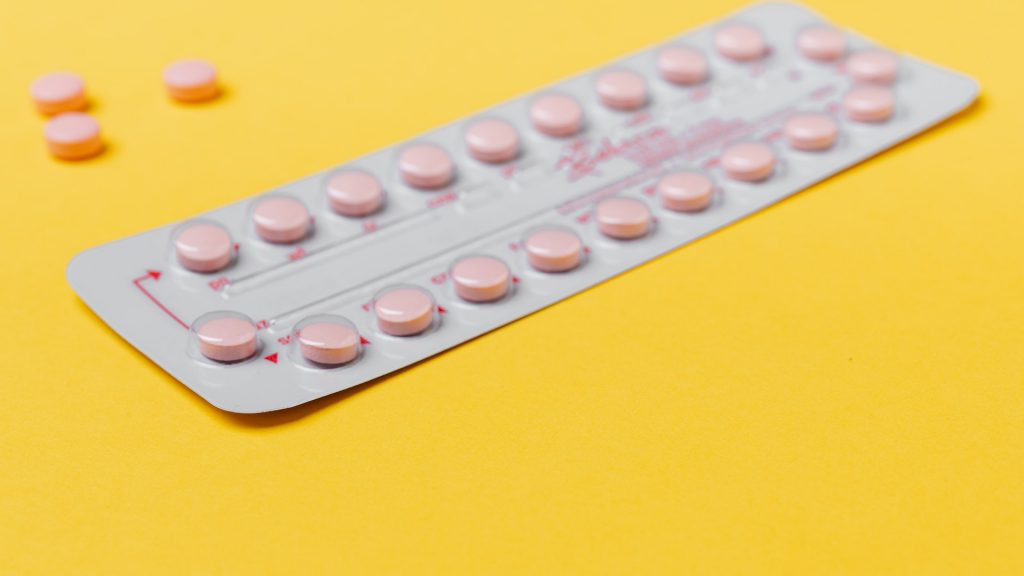
“The high level of these hormones can play a role in worsening certain conditions like thrombosis, cardiac disease and blood pressure so having a consultation will be key before initiating any new contraception method,” says Dr Gambushe.
“Go see your doctor, get a healthcare profile to find out what your risk factors are and if you’re actually a suitable candidate for the new contraceptive method that you’ve been wanting to try or that somebody else suggested.”
Read more: Is this normal: Period FAQs and their answers
Use the ‘no-gap’ method
Many women feel that they should take a break when switching between different contraceptive methods but there’s no need to wait before starting your new contraception, according to Dr Gambushe.
“Even if you were taking your old one last week or yesterday, start taking a new one as soon as possible. You don’t have to wait for any period before starting the new one,” she says.
To book an appointment with Dr Desiree Gambushe, click here.
You might experience a breakthrough bleed
During the transition between different contraceptives, breakthrough bleeding is very common, says Dr Gambushe.
“Certain contraceptive methods like the Implanon, can cause you to bleed for up to a month at a time. Fortunately, the bleeding is usually not heavy,” she says. However, if your breakthrough bleed has been going on for longer and you are feeling uncomfortable with it, you can check with your doctor who can advise you on what to do.
“Breakthrough bleeding is common and it should settle on its own. When you start seeing bleeding with clots or other some accompanying symptoms, like pelvic masses, severe pelvic pain, severe headaches, and/or additional discharge, that’s when I would definitely say go to your doctor.”
If the treatments don’t make the breakthrough bleeding subside, you should then re-look the contraception and consider different options.
Read more: Breakthrough bleeding or spotting: What it is and how long it should last
Side-effects depend on your contraception – and your body
Everyone is different and the way our bodies react to new medications and treatments will vary. That’s because different side-effects may be influence by your unique genetics. You might experience headaches, mood swings, lowered or heightened libido and, as previously mentioned, breakthrough bleeding.
“Breasts can be affected – they can feel a little bit tender or harder as well,” says Dr Gambushe. You might also experience weight loss or weight gain from the new contraception.
Use the double-barrier method
“Try to avoid having any unprotected sex within the first two weeks of starting,” says Dr Gambushe. If you do have sex, always use condoms or another method of protection aside from your contraception.
“There have been quite a few situations where patients came in and get their new contraceptive method of choice. Then they came back a few weeks later, after finding out that they’re pregnant,” she says. This can happen because you’ve been ovulating and didn’t give the new contraception enough time to start working.

Read more: Here’s why our at-home HPV test kit is a total game-changer









